COVID-19: FAQs for Organizational Leaders in the DMV
COVID-19 is a rapidly evolving situation. Below you will find quick answers to the top questions we have heard from members over the past week. We will continue to monitor the situation closely and release new information when possible.
Many of these questions were raised on a Board of Trade briefing call on March 5 with Dr. Michael J. Manyak, MD, FACS, Global Urology Medical Director at GlaxoSmithKline. Below is a summary of that Q&A and it has been reviewed by Dr. Manyak.
Is everybody overreacting? Isn’t this just a bad flu?
COVID-19 is not the flu and should not be treated like the flu. It is more severe and has a higher fatality rate, especially for people over 60 years of age and for people with compromised immune systems and other health issues. Compounding the problem is that it spreads more quickly than the flu, putting many people in the hospital at one time. When there are not enough hospital beds, equipment, and staff to properly treat those affected, fatality rates climb higher. Overwhelmed hospitals also struggle to treat people with other conditions. Intensive care units may be forced to triage patients and deny life-saving care to some. Northern Italy is currently facing this nightmare scenario.
Slowing the spread of the disease will save lives. It will keep the number of severely affected people below the threshold of what our medical system can handle. This is the idea behind the call to “flatten the curve.”
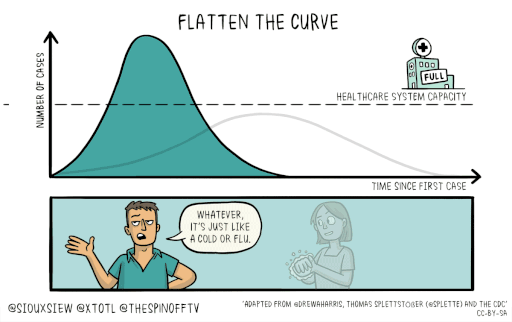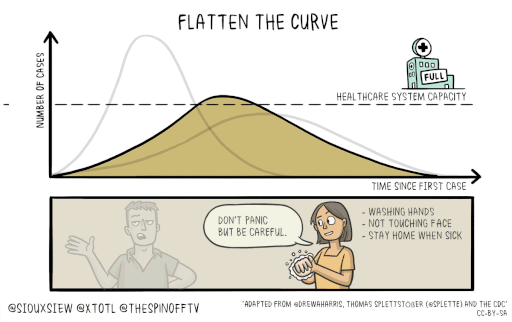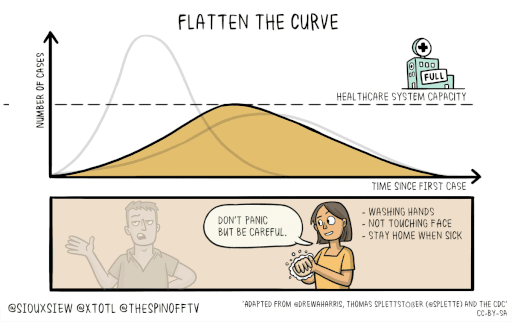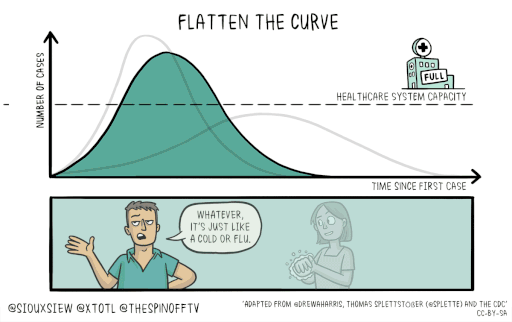
You can find more information on the COVID-19 virus on the CDC website.
What steps should I take now to protect my employees and my organization?
First, issue clear communication to employees on how to slow the spread of this disease, both within and outside your office.
- Stress the importance of following standard hygiene recommendations, such as washing hands, avoiding touching one’s face, and coughing into a tissue.
- Consider eliminating all non-essential staff travel and large meetings.
- Ask that all employees who have the symptoms of COVID-19 (fever and cough), have come into contact with someone who tested positive for COVID-19, and/or have recently visited a high-risk area stay home for 14 days.
- Employees may struggle to comply with this policy. Employers can help by enabling employees to work from home or, if that is not possible, providing paid leave. Employees should know that there will be no repercussions for taking this important precaution.
Second, start planning for a scenario where normal office operations must cease. Begin developing a business continuity plan which considers information technology needs, human resources policies, workflow adjustments, financial fallbacks, etc. (See: CDC Interim Guidance for Businesses and Employers, CDC Business Pandemic Influenza Planning Checklist, Technology Guidance for Remote Work from NTIVA, and Implications for Business from McKinsey & Company)
Lastly, consider how your organization can help the rest of the Greater Washington community should COVID-19 cause large-scale disruptions. In early 2019, this region was impacted by a prolonged government shutdown, and many types of organizations banded together to help those who were impacted. We can do that again.
What should I do if one of my employees thinks they could have COVID-19?
Instruct your employee to contact their primary care physician. If they meet the criteria for COVID-19 testing, their physician will order a test from the CDC. They should not go to the emergency department unless they are experiencing severe illness and require intensive treatment.
What should I do if one of my employees tests positive for COVID-19?
If they test positive, they should not return to your office until their primary care physician believes they are no longer contagious. You should notify all other employees who have come into contact with the infected employee and instruct them to self-quarantine for 14 days.
Am I obligated to notify the CDC or another government authority?
No. The CDC and local authorities will already know of your employee’s test results, so there is no reason to report them.
Is there a COVID-19 vaccine? What are the treatments?
There is no COVID-19 vaccine and we may not have one for another year at least. There is no specialized medicine for COVID-19, although fake medicines are being sold on the internet (do not buy them!).
Effective treatment for most cases will include the flu-recovery basics: rest, fluids, over-the-counter medicines, and hot soup. Severe cases may require hospitalization.
Should I cancel my meetings and events?
The more people who are in the same physical space at the same time, the greater the risk that a contagion will be brought into the group and spread. For this reason, many organizations are deciding to cancel or postpone large gatherings, and the DC Department of Health recommended that all gatherings over 1000 participants be postponed or cancelled. Some are moving ahead with meetings and encouraging participants to sanitize their hands and embrace contactless greetings, like waving, instead of shaking hands. Note that many organizations are disallowing staff from attending large gatherings, so if you are hosting one this spring you may see reduced attendance.
Ultimately, whether you host an event is a judgement call that depends on your risk tolerance and the risk tolerance of your attendees.
For more recommendations for event planners, see the CDC guidance.
Should I buy masks for my employees?
No. Masks should be reserved for healthcare workers and those who are already diagnosed with the virus. Wearing a mask does not reduce your risk—it only reduces supply for those who need them.
How long does the virus last on solid surfaces, like a keyboard of touchscreen?
A recent study estimates that the virus can survive on a solid surface for up to three days. For this reason, organizations should consider regularly disinfecting frequently touched surfaces in a shared office area, such as refrigerator door handles. (Note: You can find a list of COVID-19 fighting products here)
Become a member today
We need your voice at the table to make Greater Washington a place where everyone can succeed



















